
Understanding Diabetes And Managing Blood Sugar
Diabetes Management: A Clinical Guide to Blood Sugar Stability
Diabetes is not merely a “blood sugar problem”—it is a complex metabolic breakdown in how the body processes energy. Whether the issue is an autoimmune destruction of insulin-producing cells (Type 1) or a cellular resistance to insulin (Type 2), the systemic impact on the vascular and nervous systems is profound.
Medical Disclaimer: This content is for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any medical condition.
 Figure 1: How food choices shape blood sugar: sugary foods trigger rapid spikes, while whole foods support steadier, healthier glucose levels.
Figure 1: How food choices shape blood sugar: sugary foods trigger rapid spikes, while whole foods support steadier, healthier glucose levels.
🍎 The Food–Blood Sugar Connection
Every meal sends a signal to your metabolism.
Carbohydrates—especially refined ones—break down into glucose, the body’s main fuel.
When glucose enters the bloodstream, the pancreas releases insulin, guiding that sugar into cells for energy or storage.
⚖️ When Balance Breaks
Highly processed foods—white bread, sugary drinks, pastries—cause rapid spikes in blood sugar.
These spikes trigger large insulin surges, often followed by a crash that leaves you tired and hungry again.
Over time, repeated surges can lead to insulin resistance, where cells stop responding properly, forcing the pancreas to work harder.
🌿 The Steady Path
Whole foods—vegetables, beans, lean proteins, and slightly under‑ripe fruit—digest more slowly.
They create gentle glucose curves, helping maintain steady energy and protecting blood vessels and nerves.
Fiber acts like a brake pedal, slowing absorption and reducing inflammation.
🧠 Why It Matters
Stable blood sugar supports clear thinking, mood, and long‑term brain health.
Emerging research links metabolic stability to lower risk of Alzheimer’s and other age‑related conditions.
Key takeaway: Food isn’t just fuel—it’s a daily conversation with your metabolism.
Choose meals that keep that conversation calm, steady, and supportive.
 Figure 1: The Standard American Diet (SAD) is characterized by a high intake of processed foods, sugars, and unhealthy fats. Junk food meals are common in the U.S. and contribute to obesity, heart disease, and diabetes.
Figure 1: The Standard American Diet (SAD) is characterized by a high intake of processed foods, sugars, and unhealthy fats. Junk food meals are common in the U.S. and contribute to obesity, heart disease, and diabetes.
The Statistics of the “SAD” Reality
The Standard American Diet (SAD) isn’t just a lifestyle choice; it’s a primary driver of the current metabolic crisis.
- The Impact: According to the CDC, over 38 million Americans have diabetes, and approximately 98 million—more than 1 in 3 adults—have prediabetes.
- Racial Disparities: The prevalence of diagnosed diabetes is highest among:
- American Indians/Alaska Natives (13.6%)
- Black non-Hispanics (12.1%)
- Hispanics (11.7%)
- White non-Hispanics (7.5%)
Understanding these risk factors is vital for community-specific advocacy.
Decoding the Types: More Than Just Sugar
Type 1: The Autoimmune Attack
Type 1 is an insulin-deficiency disorder. The immune system destroys the beta cells in the pancreas. Without insulin—the “key” that unlocks cells—glucose remains trapped in the bloodstream, leading to cellular starvation and systemic toxicity.
Type 2: The Resistance Factor
In Type 2, the “locks” on your cells become rusty. Your body makes insulin, but the cells ignore it (insulin resistance). This is heavily influenced by the inflammatory nature of processed fats and refined sugars.
The “Type 3” Debate: Alzheimer’s and the Brain
Emerging research often refers to Alzheimer’s as “Type 3 Diabetes.” This suggests that the brain can develop its own form of insulin resistance, contributing to plaque buildup and cognitive decline. While not an official ADA diagnosis, the link between high A1C levels and cognitive impairment is a critical area in senior health.
Why Complications Happen: The Vascular Cost
High blood sugar acts like “shards of glass” in the bloodstream, damaging the lining of your vessels.
- Nephropathy (Kidney): The kidneys’ delicate filters (nephrons) become scarred. Diabetes remains the leading cause of kidney failure in the U.S.
- Retinopathy (Eyes): Small vessels in the retina leak fluid or bleed.
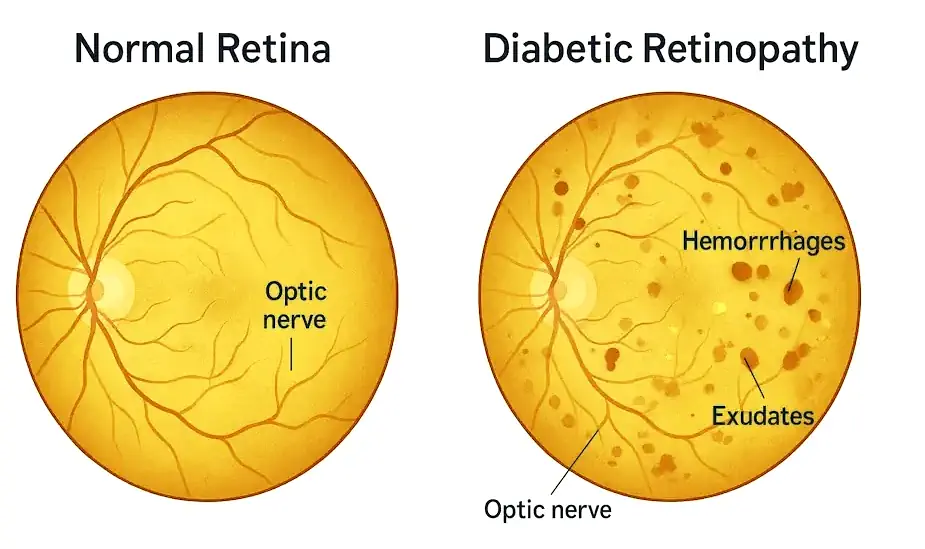 figure 3 This illustration contrasts a healthy retina with one affected by diabetic retinopathy, highlighting microaneurysms, hemorrhages, and leaky vessels caused by long‑term high blood sugar.
figure 3 This illustration contrasts a healthy retina with one affected by diabetic retinopathy, highlighting microaneurysms, hemorrhages, and leaky vessels caused by long‑term high blood sugar.
- Neuropathy (Nerves): Chronic sugar toxicity damages nerve endings, often beginning in the feet. For seniors, this is the #1 risk factor for balance issues and undiagnosed infections.
Management: Beyond “Eating Better”
Effective management requires a multidisciplinary approach:
- Glycemic Monitoring: Using a CGM (Continuous Glucose Monitor) or finger sticks to identify patterns.
- Pharmacology: From Metformin (improving insulin sensitivity) to GLP-1 agonists (regulating appetite and insulin secretion).
- The “Movement Medicine”: Exercise allows muscle contraction to pull glucose from the bloodstream without additional insulin.
📘 Personal Insight: My Triple-Threat Strategy
Author’s Note:
Living with Type 2 Diabetes is a daily negotiation. “Willpower” isn’t enough—it takes a structured medical strategy.I manage my glucose through a “Triple-Threat” approach:
- Metformin: Improves baseline insulin sensitivity.
- Ozempic (GLP-1): Regulates appetite and slows gastric emptying to prevent post-meal spikes.
- Low-Glycemic Diet: Prevents overwhelming the medications.
This combination has been a gamechanger for my A1C and reinforces the importance of transparent discussions with your endocrinologist about modern pharmacologic tools.
📝 Daily Glucose & Medication Log
| Time of Day | Glucose (mg/dL) | Medication Taken | Meal / Carbs | Energy (1–10) |
|---|---|---|---|---|
| Fasting (Morning) | Metformin? | N/A | ||
| Post-Breakfast | ||||
| Post-Lunch | ||||
| Post-Dinner | Metformin? | |||
| Weekly Ozempic Dose | Day: | Dose: | Notes: | Side effects? |
Note: Always share your logs with your endocrinologist before making dosage changes.
📘 Related Patient Resources
- Liver Health: High blood sugar drives MASLD. Learn about Liver Cirrhosis & Metabolism.
- The Vascular Link: Diabetes increases the risk of Cardiovascular Disease.
- Nutritional Strategy: How to move away from the “SAD” diet with Low-Glycemic Eating for Seniors.
📚 Fact Check & Scholarly Sources
- CDC: National Diabetes Statistics Report
- American Diabetes Association (ADA): Standards of Care in Diabetes—2024
- Mayo Clinic: Diabetic Retinopathy Pathophysiology
March 2026 Clinical Update
Current advocacy for liver health emphasizes high-protein intake (1.2–1.5 g/kg) to prevent sarcopenia.
Portal hypertension targets for esophageal or gastric varices align with maintaining systemic blood pressure below 130/80 mmHg.