Essential Insights on Flu and RSV for Tackling the Trials of the “Twin-Viremic” Season
Every year, as the temperature drops, a familiar sense of anxiety ripples through households and clinics alike. We enter the season of respiratory viruses, where the distinction between a “bad cold” and a serious medical event becomes blurry. In recent years, the spotlight has shifted from just the seasonal flu to include Respiratory Syncytial Virus (RSV).
 Understanding the structural differences between these two viruses helps scientists develop targeted vaccines and treatments.
Understanding the structural differences between these two viruses helps scientists develop targeted vaccines and treatments.
Medical Disclaimer: This content is for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any medical condition.
Understanding the nuance between flu and RSV symptoms is not just a matter of curiosity—it is a critical tool for patient advocacy. When you walk into a doctor’s office or an urgent care center, being able to articulate specific symptoms and understand the diagnostic process can significantly improve the quality of care you receive.
This guide aims to demystify these pathogens, explore the current treatment landscape, and look ahead at the future of respiratory medicine.
The Biological Profile: What Are We Dealing With?
While both are respiratory viruses, Influenza and RSV belong to different viral families. Influenza (the flu) is primarily caused by Influenza A and B viruses, known for their ability to mutate rapidly—which is why we need a new vaccine every year.
RSV, on the other hand, is a member of the Pneumoviridae family. While historically viewed as a childhood disease, we now recognize it as a major threat to older adults and those with compromised immune systems. Both viruses target the respiratory tract, but they do so with different “signatures.”
Identifying the Enemy: Understanding Flu and RSV Symptoms
The biggest hurdle for patients is that these viruses often overlap. However, observing the “onset” and “type” of discomfort can provide clues.
The Flu Signature
The flu typically hits like a freight train. One hour you feel fine; the next, you are shivering under three blankets with a high fever. Common symptoms shared by both include cough and congestion, but the flu is uniquely characterized by:
- High Fever: Often exceeding 102°F (38.88°C).
- Myalgia: Severe muscle and body aches that make moving a chore.
- Prostration: A level of fatigue that is often described as “complete exhaustion.”
The RSV Signature
In contrast, RSV often begins more like a standard cold but migrates deeper into the chest. For many adults, RSV presents as a persistent, wheezing cough. In the elderly, RSV can lead to severe secondary infections like pneumonia more rapidly than the flu might in a healthy individual.
A primary differentiator is the presence of wheezing. RSV causes inflammation in the small airways (bronchioles), leading to a whistling sound during breathing that is less common in uncomplicated influenza.
From Swabs to Solutions: Diagnostic Testing
To facilitate better healthcare conversations, it helps to know what happens after the nasal swab.
- RADTs (Rapid Antigen Diagnostic Tests): These are the “quick tests” often used in clinics. They provide results in 15 minutes but have a higher rate of false negatives.
- Molecular Assays (PCR): This is the gold standard for diagnostic testing. PCR tests look for the viral genetic material. They are much more sensitive and can distinguish between Influenza A, Influenza B, RSV, and COVID-19 in a single “multiplex” swab.
Pro-Tip: Knowing to ask for a “multiplex PCR” can save you time and multiple trips to the clinic, especially if you belong to a high-risk group.
Current Antiviral Treatments and Management
Once a diagnosis is confirmed, the clock starts ticking. For the flu, antiviral treatments like oseltamivir (Tamiflu) or baloxavir marboxil (Xofluza) are most effective when started within 48 hours of symptom onset.
For RSV, the treatment for most adults remains “supportive care”—hydration, rest, and fever management. However, for older adults, we have seen a revolution in vaccine efficacy and monoclonal antibody treatments (like Nirsevimab) that provide “passive immunity.”
Case Study: The “Just a Cold” Fallacy
Margaret, a 72-year-old with mild asthma, began feeling congested in late November. Assuming it was a common cold, she stayed home. By day four, her symptoms escalated into severe wheezing and cyanosis (a blue tint around the fingernails). A multiplex PCR confirmed RSV. Because her asthma was already taxing her lungs, she required three days of supplemental oxygen. Margaret’s experience highlights the importance of early diagnostic testing for those with underlying conditions.
The Future: A Proactive Defense
We are entering a “Golden Age” of vaccinology. mRNA technology is being leveraged to create combination vaccines—a single shot covering Flu, RSV, and COVID-19. Furthermore, researchers are investigating “universal flu vaccines” that target the “stalk” of the virus, potentially ending the need for annual shots.
Conclusion: Empowering the Patient
Navigating respiratory season requires a shift from passive patient to active participant. By recognizing the nuances of symptoms and understanding diagnostic options, you can engage in more productive dialogues with your physician.
Don’t be afraid to ask: “Which test are we using?” or “Am I a candidate for antivirals?” Knowledge is the best defense.
Glossary of Terms
- Myalgia: Muscle pain or soreness, often widespread during viral infections.
- Bronchiolitis: Inflammation of the smallest air passages in the lungs.
- Multiplex PCR: A laboratory technique that detects multiple different viruses from a single sample.
- Monoclonal Antibodies: Proteins that mimic the immune system’s ability to fight pathogens.
- Passive Immunity: Protection provided by antibodies produced outside the body.
- Neuraminidase Inhibitors: Drugs (like Tamiflu) that block the enzyme viruses use to spread from cell to cell.
Frequently Asked Questions
Can I have the flu and RSV at the same time?
Yes. This is known as a co-infection. Healthcare providers manage this by treating symptoms of both and using antivirals specifically for the flu component.
Why isn’t there a “Tamiflu” for RSV yet?
RSV has a different structure than the flu. While we have ribavirin for severe hospital cases, oral pills for general use are currently in clinical trials.
Does the flu shot protect me against RSV?
No. They are entirely different viruses. You need the specific RSV vaccine (recommended for adults 60+) to gain protection against RSV.
Professional Sources
- “Influenza Antiviral Medications: Summary for Clinicians” - CDC, 2025.
- “Tamiflu Information” - Drugs.com, 2025.
- Ascough, S. et al. “Induction and Subversion of Human Protective Immunity.” Frontiers in Immunology, 2018.
- “RSV in Adults” - CDC, 2025.
### 💪 Sarcopenia (Muscle Health)
Definition: Age-related loss of muscle mass and strength.
### 💪 age-related muscle loss (Muscle Health)
Definition: Age-related loss of muscle mass and strength.
### 💪 muscle wasting in older adults (Muscle Health)
Definition: Age-related loss of muscle mass and strength.
### 💪 loss of strength with aging (Muscle Health)
Definition: Age-related loss of muscle mass and strength.
### 🫀 high blood pressure condition (Heart and Circulation)
Definition: High blood pressure.
### 🫀 elevated blood pressure levels (Heart and Circulation)
Definition: High blood pressure.
### 🫀 blood pressure too high (Heart and Circulation)
Definition: High blood pressure.
### 🧠 Delirium (Cognitive Health)
Definition: A sudden change in mental status.
### 🧴 Psoriasis (Skin and Autoimmune)
Definition: A chronic autoimmune skin condition that causes red, scaly patches.
### 🧪 Chlorine (Skin and Autoimmune)
Definition: A disinfectant used in pools that may irritate sensitive skin.
### 🧂 Magnesium (Skin and Autoimmune)
Definition: A mineral that may reduce inflammation and soothe psoriatic skin.
### 🦴 Arthritis (Bone and Joint Health)
Definition: Joint inflammation that causes pain and stiffness.
### 🦴 Osteoarthritis (Bone and Joint Health)
Definition: A degenerative joint condition caused by cartilage breakdown.
### 🦴 Rheumatoid Arthritis (Bone and Joint Health)
Definition: An autoimmune disorder that causes joint inflammation.
### 🦴 Osteoporosis (Bone and Joint Health)
Definition: A condition where bones become weak and brittle.
### 🦴 Bone Density (Bone and Joint Health)
Definition: A measure of bone strength.
### 🧠 Dementia (Cognitive Health)
Definition: A group of conditions affecting memory, thinking, and behavior.
### 🧠 Alzheimers Disease (Cognitive Health)
Definition: The most common form of dementia, affecting memory and cognition.
### 🧠 Cognitive Decline (Cognitive Health)
Definition: A decrease in memory, attention, or decision-making abilities.
### 🧠 sudden confusion episode (Cognitive Health)
Definition: A sudden change in mental status.
### 🧠 acute mental status change (Cognitive Health)
Definition: A sudden change in mental status.
### 🧠 rapid onset confusion (Cognitive Health)
Definition: A sudden change in mental status.
### ❤️ Hypertension (Heart and Circulation)
Definition: High blood pressure that increases risk of heart disease.
### ❤️ Hypotension (Heart and Circulation)
Definition: Low blood pressure that may cause dizziness or fainting.
### ❤️ Atherosclerosis (Heart and Circulation)
Definition: Hardening or narrowing of the arteries due to plaque buildup.
### 🧠 Stroke (Heart and Circulation)
Definition: A condition where blood flow to the brain is interrupted.
### 🧠 TIA (Heart and Circulation)
Definition: A transient ischemic attack, often called a mini-stroke.
### ❤️ Heart Failure (Heart and Circulation)
Definition: A condition where the heart cannot pump blood effectively.
### ❤️ Arrhythmia (Heart and Circulation)
Definition: An irregular heartbeat pattern.
### ❤️ Atrial Fibrillation (Heart and Circulation)
Definition: A common arrhythmia that increases stroke risk.
### 🌬️ COPD (Lung and Breathing)
Definition: A chronic lung disease that makes breathing difficult.
### 🌬️ Emphysema (Lung and Breathing)
Definition: A lung condition where air sacs are damaged.
### 🌬️ Chronic Bronchitis (Lung and Breathing)
Definition: Long-term inflammation of the airways.
### 💪 Sarcopenia (Mobility and Strength)
Definition: Age-related loss of muscle mass and strength.
### 💪 Frailty (Mobility and Strength)
Definition: A condition of reduced strength and resilience in older adults.
### ⚠️ Fall Risk (Mobility and Strength)
Definition: The likelihood of experiencing a fall due to balance or mobility issues.
### 🦶 Peripheral Neuropathy (Mobility and Strength)
Definition: Nerve damage causing numbness or tingling in the limbs.
### 🚽 Incontinence (Bladder and Bowel Health)
Definition: Loss of bladder or bowel control.
### 🚽 UTI (Bladder and Kidney Health)
Definition: A urinary tract infection affecting the bladder or kidneys.
### 👁️ Glaucoma (Eye Health)
Definition: An eye condition that can damage the optic nerve.
### 👁️ Cataracts (Eye Health)
Definition: Clouding of the eye’s lens that affects vision.
### 👁️ Macular Degeneration (Eye Health)
Definition: A condition affecting central vision.
### 👂 Hearing Loss (Hearing and Ear Health)
Definition: Reduced ability to hear sounds clearly.
### 👂 Tinnitus (Hearing and Ear Health)
Definition: Ringing or buzzing in the ears.
### 🔥 Chronic Pain (Pain and Inflammation)
Definition: Long-lasting pain that persists beyond normal healing.
### 🔥 Inflammation (Pain and Inflammation)
Definition: The body's response to injury or infection.
### 🔥 Inflammatory Response (Pain and Inflammation)
Definition: The body's reaction to harmful stimuli.
### 🧬 Autoimmune Disease (Immune System and Infection)
Definition: A condition where the immune system attacks the body.
### 🧬 Immune System (Immune System and Infection)
Definition: The body's defense system against illness.
### 🧫 Pathogen (Immune System and Infection)
Definition: A microorganism that can cause disease.
### 🦠 Virus (Immune System and Infection)
Definition: A tiny infectious agent that replicates inside living cells.
### 🦠 Bacteria (Immune System and Infection)
Definition: Single-celled organisms that can be helpful or harmful.
### 🍄 Fungus (Immune System and Infection)
Definition: A type of organism that includes molds and yeasts.
### 🧬 Antibody (Immune System and Infection)
Definition: A protein produced by the immune system to fight infections.
### 🧬 Antigen (Immune System and Infection)
Definition: A substance that triggers an immune response.
### 💢 Myalgia (Immune System and Infection)
Definition: Muscle pain or soreness, often widespread during viral infections.
### 🌬️ Bronchiolitis (Immune System and Infection)
Definition: Inflammation of the smallest air passages in the lungs, common in RSV cases.
### 🧪 Multiplex PCR (Immune System and Infection)
Definition: A laboratory technique that can detect multiple viruses from a single sample simultaneously.
### 🧬 Monoclonal Antibodies (Immune System and Infection)
Definition: Laboratory-made proteins that mimic the immune system’s ability to fight harmful pathogens.
### 🛡️ Passive Immunity (Immune System and Infection)
Definition: Protection against disease provided by antibodies produced outside the body.
### 💊 Neuraminidase Inhibitors (Immune System and Infection)
Definition: A class of drugs that block the enzyme viruses use to spread.
### 💧 Dehydration (Hydration and Nutrition)
Definition: A condition caused by insufficient fluid intake.
### 🥗 Malnutrition (Hydration and Nutrition)
Definition: Lack of proper nutrients for health.
### 🩸 Anemia (Hydration and Nutrition)
Definition: A condition where the body lacks enough healthy red blood cells.
### 🍬 disaccharide (Nutrition)
Definition: A carbohydrate made of two linked sugar molecules.
### 🍭 five‑carbon sugar alcohol (Nutrition)
Definition: A five‑carbon sugar alcohol used as a low-calorie sweetener.
### 🍭 xylitol (Nutrition)
Definition: A sugar alcohol commonly used as a sweetener that does not raise blood glucose significantly.
### 📉 low glycemic index (Nutrition)
Definition: A measure of how slowly or quickly a food raises blood glucose.
### ⚖️ pH balance (Dental Health)
Definition: The overall balance of acidity and alkalinity in the mouth.
### 🦷 tooth decay (Dental Health)
Definition: Damage to teeth caused by acids produced by bacteria.
### ✨ dental benefits (Dental Health)
Definition: Advantages to oral health such as reduced cavity risk or improved enamel strength.
### 🧪 phosphate (Dental Health)
Definition: A mineral important for tooth structure and enamel strength.
### 🦠 Streptococcus mutans (Dental Health)
Definition: A common oral bacterium associated with cavity formation.
### 🔄 remineralization (Dental Health)
Definition: The natural process of restoring minerals to tooth enamel.
### 💧 saliva (Dental Health)
Definition: Fluid produced in the mouth that protects teeth and supports digestion.
### 🦠 plaque (Dental Health)
Definition: A sticky film of bacteria that forms on teeth.
### 🦷 dental health (Dental Health)
Definition: The overall condition of teeth, gums, and oral tissues.
### 🛡️ tooth enamel (Dental Health)
Definition: The hard outer surface of the tooth that protects against decay.
### 🦴 osteoporosis (Bone Health)
Definition: A condition where bones become weaker and more prone to fracture.
### 🔨 osteoclasts (Bone Health)
Definition: Cells that break down old bone tissue as part of natural bone remodeling.
### 🦴 bones (Bone Health)
Definition: The rigid structures that support the body and protect organs.
### ⚙️ calcium (Bone Health)
Definition: A mineral essential for bone strength and many body functions.
### 🌿 gut health (Wellness)
Definition: The condition of the digestive system and its influence on overall well-being.
### ⏳ longevity (Wellness)
Definition: Long-term health and lifespan influenced by genetics, lifestyle, and environment.
### 🧬 Genomics (Wellness)
Definition: The study of genes and how they influence health and traits.
### 🌱 healthy choices (Wellness)
Definition: Actions that support better health and reduce future risk.
### 🛡️ preventive medicine (Wellness)
Definition: An approach focused on reducing disease risk before it develops.
### 💡 modern technology (Wellness)
Definition: Tools and innovations that enhance modern health practices.
### ✨ imagination (General)
Definition: The ability to form new ideas or concepts.
### 🌿 Clinical Insights (Wellness)
Definition: Insights gained from clinical observation or research that help guide health decisions.
### 🦷 bacteria (Dental Health)
Definition: Microorganisms that can live in the mouth and influence oral health.
### 🦷 dental caries (Dental Health)
Definition: Damage to teeth caused by acids produced by bacteria.
### 🦷 cavities (Dental Health)
Definition: Damage to teeth caused by acids produced by bacteria.
### ⚡ Metabolism (Metabolism and Endocrine)
Definition: The body's process of converting food into energy.
### 🦋 Thyroid Disorder (Metabolism and Endocrine)
Definition: Conditions affecting thyroid hormone production.
### 🦋 Hypothyroidism (Metabolism and Endocrine)
Definition: Low thyroid hormone levels.
### 🦋 Hyperthyroidism (Metabolism and Endocrine)
Definition: High thyroid hormone levels.
### 🩸 Cholesterol (Metabolism and Endocrine)
Definition: A fatty substance in the blood that can affect heart health.
### 🩸 Triglycerides (Metabolism and Endocrine)
Definition: A type of fat found in the blood.
### 🩸 Blood Glucose (Metabolism and Endocrine)
Definition: The amount of sugar in the bloodstream.
### 🩸 Type 2 Diabetes (Metabolism and Endocrine)
Definition: A condition where the body struggles to regulate blood sugar.
### 🩸 Insulin Resistance (Metabolism and Endocrine)
Definition: A condition where cells do not respond well to insulin.
### 💛 Caregiver Stress (Aging and Caregiving)
Definition: Emotional and physical strain experienced by caregivers.
### 📄 Advance Directive (Aging and Caregiving)
Definition: A legal document outlining healthcare wishes.
### ⚡ Acute (General Health)
Definition: A condition with sudden onset and short duration.
### 🕒 Chronic (General Health)
Definition: A long-lasting or persistent condition.
### 🧪 Biopsy (General Health)
Definition: A procedure where a small tissue sample is examined.
### 🔍 Diagnosis (General Health)
Definition: The process of identifying a medical condition.
### 📈 Prognosis (General Health)
Definition: The expected outcome of a condition.
### ⚠️ Symptom (General Health)
Definition: A physical or mental sign of a condition.
### ⚠️ Risk Factor (General Health)
Definition: A trait or behavior that increases disease likelihood.
### 💊 Treatment (General Health)
Definition: Actions taken to manage or improve a condition.
### 💬 Therapy (General Health)
Definition: A treatment method for physical or mental health.
### 🧬 Hormone (General Health)
Definition: A chemical messenger that regulates body functions.
### 🧬 Genetics (General Health)
Definition: The study of inherited traits and DNA.
### 🧬 Adenocarcinoma (Cancer Types)
Definition: A cancer that begins in gland-forming tissues found throughout the body.
### 🩺 Cholangiocarcinoma (Cancer Types)
Definition: Cancer that develops in the bile ducts.
### 🌕 Jaundice (Symptoms)
Definition: Yellowing of the skin and eyes caused by a buildup of bilirubin.
### 🔪 Resection (Procedures)
Definition: Surgical removal of part of an organ or tissue.
### 🌿 Complementary Therapy (Treatment Approaches)
Definition: Treatments used alongside standard medical care to support well-being.
### 🧬 Bioavailability (General Health)
Definition: it is the fraction or percentage of an administered dose that reaches the bloodstream unchanged.
### 🧬 Oxidative Stress (General Health)
Definition: An imbalance where harmful, unstable molecules called free radicals (Reactive Oxygen Species - ROS) overwhelm the body's antioxidant defenses, causing damage to cells, proteins, and DNA, contributing to aging and chronic diseases like cancer, diabetes, and heart disease.
### 🧬 Telomeres (Longevity)
Definition: Cap the ends of chromosomes, acting like plastic tips on shoelaces to prevent them from fraying, sticking together, or being recognized as damaged DNA.
### 😒 Cortisol (Hormones)
Definition: a vital steroid hormone from your adrenal glands that manages stress, metabolism (blood sugar, fats, proteins), blood pressure, and inflammation
### 🔋 Mitochondria (Cellular Health)
Definition: The 'powerhouses' of the cell that convert nutrients into ATP (energy) to fuel all bodily functions.
### 🧠 Neuroplasticity (Neurology)
Definition: The brain’s lifelong ability to reorganize itself by forming new neural connections in response to learning or recovery from injury.
### 🦠 Microbiome (Systemic Health)
Definition: The community of microorganisms living in the gut that regulates digestion, immunity, and metabolic health.
### 🔥 Inflammaging (Cellular Health)
Definition: A state of persistent, low-grade chronic inflammation that develops with age and drives many age-related diseases.
### ⚡ Free Radical (Cellular Health)
Definition: Unstable molecules that can damage cell structures and DNA, a process known as oxidative stress.
### 🛡️ Cognitive Reserve (Neurology)
Definition: The brain's ability to find alternative ways to function and maintain mental agility despite damage or age-related changes.
### 🍇 Polyphenols (Nutrition)
Definition: Beneficial plant compounds with antioxidant properties that protect cells from damage and support heart and brain health.
### 🦴 Bone Density (Musculoskeletal)
Definition: A measurement of the amount of minerals (like calcium) in bone tissue, used to determine bone strength and fracture risk.
### ♻️ Autophagy (Cellular Health)
Definition: The body's 'self-cleaning' process where cells break down and recycle their own damaged components to maintain health.
### 📨 Cytokines (Immune System)
Definition: Small proteins released by cells that act as chemical messengers to coordinate the body's immune response and inflammation.
### 🌅 Circadian Rhythm (Lifestyle)
Definition: The internal 24-hour clock that regulates sleep, hormone release, and metabolism based on light and darkness.
### ⚖️ Homeostasis (Systemic Health)
Definition: The state of steady internal physical and chemical balance maintained by living systems for optimal survival.
### 🧠 Amyloid Plaques (Neurology)
Definition: Sticky protein buildups that collect between nerve cells in the brain, often associated with the progression of Alzheimer’s disease.
### 🧬 telomere (Biology)
Definition: Protective DNA caps at chromosome ends that shorten with each cell division, impacting cellular aging.
### ⚡ oxidative stress (Biology)
Definition: An imbalance between free radicals and antioxidants that can damage cells and accelerate aging.
### 🌐 systemic (Medicine)
Definition: Affecting the entire body or multiple organ systems, often involving widespread immune or inflammatory responses.
### 📚 hippocampal (Neurology)
Definition: Relating to the hippocampus, a memory‑forming brain region vulnerable to stress and aging.
### 🎭 amygdala (Neurology)
Definition: A brain structure that processes fear, threat, and emotional significance, shaping stress responses.
### 🧬 human chimera definition (Genetics)
Definition: A condition where a person has two sets of DNA.
### 🧬 dual genome condition (Genetics)
Definition: A condition where a person has two sets of DNA.
### 🧬 microchimerism explained (Genetics)
Definition: Presence of a small number of cells from another individual.
### 🧬 fetal cells in mother (Genetics)
Definition: Presence of a small number of cells from another individual.
### 🧠 glymphatic system function (Brain Health)
Definition: A sleep-driven system that clears waste from the brain.
### 🧠 sleep-driven brain detox (Brain Health)
Definition: A sleep-driven system that clears waste from the brain.
### 🦠 gut microbiome diversity (Digestive Health)
Definition: The community of microorganisms living in the human gut.
### 🦠 gut-brain axis connection (Digestive Health)
Definition: The community of microorganisms living in the human gut.
### 🧩 placebo neurobiology (Mind-Body Health)
Definition: A beneficial response to an inactive treatment due to expectation.
### 🧩 expectation-driven healing (Mind-Body Health)
Definition: A beneficial response to an inactive treatment due to expectation.
### 😊 endogenous opioid system (Pain and Mood)
Definition: Natural pain-relieving chemicals produced by the body.
### 😊 natural endorphin boosters (Pain and Mood)
Definition: Natural pain-relieving chemicals produced by the body.
### 🦴 bone remodeling cycle (Bone and Joint Health)
Definition: The continuous cycle of bone breakdown and rebuilding.
### 🦴 osteoblast vs osteoclast (Bone and Joint Health)
Definition: The continuous cycle of bone breakdown and rebuilding.
### 🧬 epigenetic inheritance (Genetics)
Definition: Changes in gene expression without altering DNA sequence.
### 🧬 environmental epigenetics (Genetics)
Definition: Changes in gene expression without altering DNA sequence.
### ⚡ bioelectric healing signals (Regeneration)
Definition: Electrical signals that guide healing and tissue repair.
### ⚡ voltage-guided tissue repair (Regeneration)
Definition: Electrical signals that guide healing and tissue repair.
### ❄️ induced human torpor (Future Medicine)
Definition: Research exploring whether humans can enter a low-metabolic torpor state.
### ❄️ metabolic slowing research (Future Medicine)
Definition: Research exploring whether humans can enter a low-metabolic torpor state.
### 🩸 A1c (Diabetes Basics)
Definition: A blood test showing your average blood sugar over about three months.
### 🧪 C-Peptide (Biomarkers)
Definition: A marker that helps show how much insulin your body is producing.
### 📈 CGM (Devices)
Definition: A wearable device that tracks glucose levels throughout the day and night.
### 🌅 Dawn Phenomenon (Glucose Patterns)
Definition: A natural early-morning rise in blood sugar caused by hormone changes.
### ⏱️ Fasting Glucose (Biomarkers)
Definition: Your blood sugar level after not eating for at least eight hours.
### 🥣 Gastroparesis (Complications)
Definition: Slow stomach emptying that can cause nausea, bloating, or early fullness.
### 💊 GLP-1 Medication (Medications)
Definition: A type of diabetes medicine that helps control appetite and blood sugar.
### 📈 Hyperglycemia (Symptoms)
Definition: High blood sugar that may cause thirst, fatigue, or frequent urination.
### 📉 Hypoglycemia (Symptoms)
Definition: Low blood sugar that may cause shakiness, sweating, or confusion.
### 🧬 Insulin Resistance (Metabolic Health)
Definition: When the body has trouble using insulin effectively, causing higher glucose levels.
### 🔥 Ketones (Metabolic Health)
Definition: Chemicals made when the body burns fat for energy; high levels can be dangerous.
### 💊 Metformin (Medications)
Definition: A common first-line diabetes medication that helps reduce glucose production in the liver.
### 🦶 Neuropathy (Complications)
Definition: Nerve damage that can cause tingling, numbness, or burning sensations.
### 🍽️ Postprandial Glucose (Biomarkers)
Definition: Your blood sugar level after eating a meal.
### 🚰 SGLT2 Inhibitor (Medications)
Definition: A medication that helps the kidneys remove extra glucose through urine.
### 🍎 oxalates (Nutrition)
Definition: Naturally occurring compounds in plants that can bind to minerals such as calcium.
### 🍎 oxalic acid (Nutrition)
Definition: Naturally occurring compounds in plants that can bind to minerals such as calcium.
### 💧 calcium oxalate kidney stones (Kidney Health)
Definition: A type of kidney stone formed when calcium binds with oxalate.
### 💧 oxalate kidney stones (Kidney Health)
Definition: A type of kidney stone formed when calcium binds with oxalate.
### 🌿 Oxalobacter formigenes (Gut Health)
Definition: A gut bacterium that helps break down oxalates in the digestive tract.
### 🍎 high-oxalate foods (Nutrition)
Definition: Foods that contain higher levels of oxalates, such as spinach, almonds, and beets.
### 🍎 low-oxalate diet (Nutrition)
Definition: A dietary pattern that limits foods high in oxalates.
### 🌿 oxalate absorption (Gut Health)
Definition: The process by which oxalates are absorbed through the digestive tract.
### ✨ oxalate sensitivity (General)
Definition: A term sometimes used to describe symptoms people attribute to changes in oxalate intake.
### ✨ oxalate intolerance (General)
Definition: A term sometimes used to describe symptoms people attribute to changes in oxalate intake.
### 🏃 aerobic exercise (Exercise)
Definition: Movement that increases heart rate and breathing, such as walking or swimming. Supports heart, lung, and brain health.
### 💪 strength training (Exercise)
Definition: Exercises that build muscle and bone strength using resistance bands, weights, or bodyweight. Helps prevent falls.
### ⚖️ balance training (Exercise)
Definition: Exercises that improve stability and coordination, reducing fall risk. Includes tai chi and heel-to-toe walking.
### 🤸 flexibility training (Exercise)
Definition: Stretching movements that improve range of motion and reduce stiffness.
### 🌿 low-impact exercise (Exercise)
Definition: Movement that reduces stress on joints, such as swimming, cycling, or chair aerobics.
### 🪑 chair aerobics (Exercise)
Definition: Seated or supported aerobic movements designed for seniors with limited mobility.
### 🔧 functional fitness (Exercise)
Definition: Exercises that mimic everyday movements like standing, lifting, or reaching to improve independence.
### 💨 moderate-intensity exercise (Exercise)
Definition: Activity that raises heart rate but still allows conversation, such as brisk walking.
### 🔥 vigorous exercise (Exercise)
Definition: High-effort activity that significantly increases heart rate and breathing.
### ⏱️ interval training (Exercise)
Definition: Alternating short bursts of activity with rest or slower movement.
### 🏅 endurance training (Exercise)
Definition: Activities that build stamina and cardiovascular health over time.
### 🔄 mobility exercises (Exercise)
Definition: Movements that improve joint comfort and ease of motion.
### 📏 range of motion (Mobility)
Definition: How far a joint can move in each direction. Often decreases with age.
### 🚶 gait (Mobility)
Definition: The pattern of how a person walks, including speed, stride, and balance.
### 🧍 posture (Mobility)
Definition: The alignment of the body while sitting or standing. Affects balance and comfort.
### 🧘 core strength (Mobility)
Definition: Strength of the muscles in the abdomen, back, and pelvis that support stability.
### 🦴 joint mobility (Mobility)
Definition: The ability of a joint to move freely and comfortably.
### 🔁 functional mobility (Mobility)
Definition: The ability to move safely and independently during daily tasks.
### 🧍♂️ static balance (Mobility)
Definition: The ability to stay steady while standing still.
### 🚶♂️ dynamic balance (Mobility)
Definition: The ability to stay steady while moving.
### 🎯 coordination (Mobility)
Definition: The ability to move different parts of the body smoothly and efficiently.
### 🪨 stability (Mobility)
Definition: The ability to maintain control of body position during movement.
### ⚠️ fall risk (Safety)
Definition: The likelihood of losing balance or falling. Increased by weak muscles, medications, or vision changes.
### 🔥 warm-up (Safety)
Definition: Gentle movements performed before exercise to prepare muscles and reduce injury risk.
### ❄️ cool-down (Safety)
Definition: Light movement and stretching after exercise to help the body recover.
### ⛔ overexertion (Safety)
Definition: Pushing the body beyond safe limits, causing dizziness, pain, or extreme fatigue.
### 🩹 joint strain (Safety)
Definition: Stress or irritation in a joint caused by overuse or improper movement.
### 📐 proper form (Safety)
Definition: Using correct body alignment during exercise to prevent injury.
### 💧 hydration (Safety)
Definition: Maintaining adequate fluid intake before, during, and after exercise.
### 🚫 pain signal (Safety)
Definition: A warning sign from the body indicating that an exercise may be unsafe or too intense.
### 😮💨 fatigue (Safety)
Definition: A feeling of tiredness that may indicate the need for rest or lighter activity.
### 💨 shortness of breath (Safety)
Definition: Difficulty breathing during activity; may signal overexertion or a medical issue.
### 🟦 resistance band (Equipment)
Definition: A stretchy band used for strength training. Gentle on joints and ideal for seniors.
### 🏋️ dumbbells (Equipment)
Definition: Handheld weights used for strength training. Light weights are ideal for beginners.
### ⚽ stability ball (Equipment)
Definition: A large inflatable ball used for core and balance exercises.
### 🧘♀️ yoga mat (Equipment)
Definition: A cushioned mat used for stretching, yoga, and floor exercises.
### 🌀 foam roller (Equipment)
Definition: A tool used to massage muscles and improve flexibility.
### 🦯 walking poles (Equipment)
Definition: Poles used to improve stability and reduce joint impact during walking.
### 🎒 ankle weights (Equipment)
Definition: Light weights worn around the ankles to increase resistance during leg exercises.
### 🪑 chair support (Equipment)
Definition: A sturdy chair used for balance, seated exercise, or modified strength training.
### 🏃♂️ treadmill (Equipment)
Definition: A machine used for indoor walking or light jogging.
### 🔁 elliptical machine (Equipment)
Definition: A low-impact cardio machine that reduces stress on joints.
### 🥬 oxalates (Nutrition)
Definition: Naturally occurring compounds in plants that can bind to minerals such as calcium.
### 🥗 low oxalate diet (Nutrition)
Definition: A diet designed to reduce oxalate intake to help prevent kidney stone formation.
### 🦠 Oxalobacter formigenes (Bioprinting)
Definition: A helpful gut bacterium that breaks down oxalates and may reduce kidney stone risk.
### 🌾 Gluten (Nutrition)
Definition: A protein found in wheat, barley, and rye that can trigger immune reactions in susceptible individuals.
### 🌿 Villi (Gut Health)
Definition: Finger‑like projections in the small intestine that absorb nutrients.
### 🦠 Intestinal Permeability (Gut Health)
Definition: A condition where the gut lining becomes more porous, allowing particles to pass into the bloodstream.
### 🌾 Non‑Celiac Gluten Sensitivity (NCGS) (Gut Health)
Definition: A condition where gluten causes symptoms without autoimmune markers.
### 🌾 FODMAPs (Gut Health)
Definition: Fermentable carbohydrates that can mimic gluten symptoms.
### 🌾 Transglutaminase 2 (TG2) (Gut Health)
Definition: An enzyme involved in celiac autoimmune reactions.
### 🧠 Iatrophobia (Neurology)
Definition: an overwhelming and irrational dread of doctors, medical settings, or procedures.
### 🧠 Prediabetes</ (Metabolic Health)
Definition: When the body’s cells do not respond well to insulin, causing blood sugar to rise.
### 🧠 A1C/ (Metabolic Health)
Definition: A blood test that measures average blood sugar levels over the past 2–3 months
### 🧠 Fasting Glucose/ (Metabolic Health)
Definition: Blood sugar measured after not eating for at least 8 hours.
### 🧠 Neuropathy/ (Metabolic Health)
Definition: Nerve damage that can cause tingling, numbness, or burning sensations.
### 🧠 Acanthosis Nigricans/ (Metabolic Health)
Definition: Dark, velvety skin patches often linked to insulin resistance.
### 🌿 Flatulence/ (Gut Health)
Definition: The release of gas from the digestive tract
### 🌿 Fermentation/ (Gut Health)
Definition: The process where gut bacteria break down food, producing gas..
### 🌿 Lactulose/ (Gut Health)
Definition: A synthetic sugar used to help remove ammonia in liver disease.
### 🌿 Ammonia (Gut Health)
Definition: A waste product that can build up when the liver is damaged.
### 🌿 Sulfur Compounds/ (Gut Health)
Definition: Molecules responsible for the smell in some types of gas.
### 🧬 mRNA Platform (Genetics)
Definition: A technology that delivers genetic instructions to cells to trigger an immune response.
### 🧬 Neoantigen (Cancer Types)
Definition: A waste product that can build up when the liver is damaged.
### 🧬 Xenotransplantation (Treatment Approaches)
Definition: Transplanting organs from one species to another.
### 🧠 Amyloid Plaques (Neurology)
Definition: Protein deposits associated with Alzheimer’s disease.
### 🤖 AI Diagnostics (Diagnostics)
Definition: Computer systems that analyze medical data to assist clinicians.
### 🧬 Bioprinting (General)
Definition: 3D printing of biological tissues using living cells.
### 🌍 Carbon Footprint (Environment)
Definition: Total greenhouse gases caused by an individual or household.
### 🌍 AI Diagnostics (Nutrition)
Definition: Diet choices that support health and reduce emissions
### 🌍 Energy Efficiency (Environment)
Definition: Using less energy for the same service.
### 🌍 Environmental Sustainability (Environment)
Definition: Protecting natural systems for long‑term health.
### 🌍 Biophilic Routines (Environment)
Definition: Habits that increase connection with nature.
### 🌍 Low‑Tox Home Swap (Environment)
Definition: Replacing products with safer alternatives.
### 👴🏻 Healthy Aging (Aging)
Definition: Maintaining physical, mental, and social well‑being as you grow older.
### 💪🏻 Resistance Training (Exercise)
Definition: Exercises that strengthen muscles using weights or body resistance.
### 🧠 Executive Function (Neurology)
Definition: Brain skills used for planning, focus, and decision‑making.
### 🧠 Intrinsic Capacity (Neurology)
Definition: Maintaining physical, mental, and social well‑being as you grow older.
### 💪🏻 Balance Training (Exercise)
Definition: Exercises that improve stability and prevent falls.
### 🧑🏻⚕️ Preventive Care (General Health)
Definition: Actions taken to avoid illness rather than treat it later.
### 🧬 Epigenetic Drift (Aging Science)
Definition: Gradual changes in DNA methylation patterns that alter gene activity and contribute to aging
### ⚡ Mitochondrial Dysfunction (Cellular Health)
Definition: A decline in mitochondrial efficiency that reduces cellular energy production and accelerates aging.
### ♻️ Lysosomal Cleanup (Cellular Cleanup)
Definition: The cell’s recycling process that removes damaged proteins and debris to maintain healthy function.
### 🔥 Inflammaging (Inflammation)
Definition: Chronic, low‑grade inflammation that increases with age and contributes to many age‑related diseases.
### ⏳ Biological Age (Longevity)
Definition: A measure of cellular aging based on biomarkers, often differing from chronological age.
### 🧠 Hypothalamic Signaling (Brain & Hormones)
Definition: Hormonal and inflammatory signals from the hypothalamus that influence metabolism, stress responses, and aging.
### 💵 Premium (Medicare)
Definition: The monthly amount you pay for Medicare coverage.
### 📉 Deductible (Medicare)
Definition: The amount you pay out of pocket before Medicare begins covering services.
### ⚖️ Coinsurance (Insurance)
Definition: A percentage of costs you pay after meeting your deductible.
### 💊 Formulary (Medicare)
Definition: A list of prescription drugs covered by a Medicare Part D plan.
### 🏥 Network (Insurance)
Definition: The group of doctors and facilities contracted with a Medicare Advantage plan.
### 🛡️ Medigap (Medicare)
Definition: Supplemental insurance that helps cover costs not paid by Original Medicare.
### 🧬 Endocrine System (Endocrinology)
Definition: The network of glands that produce hormones regulating metabolism, growth, and stress response.
### ⚖️ Hormone Imbalance (Endocrinology)
Definition: A condition where hormone levels are too high or too low, affecting energy, weight, and mood.
### 🔥 Metabolic Disorders (Endocrinology)
Definition: Conditions affecting how the body converts food into energy, such as diabetes or lipid disorders.
### 🦋 Thyroid Health (Endocrinology)
Definition: The function of the thyroid gland in regulating metabolism, energy, and body temperature.
### ⚡ Adrenal Glands (Endocrinology)
Definition: Glands that produce cortisol and adrenaline to regulate stress, blood pressure, and metabolism.
### 🔄 GLUT4 (Endocrinology)
Definition: A protein that transports glucose into muscle and fat cells in response to insulin or exercise.
### 😊 Endorphins (Endocrinology)
Definition: Neurochemicals that alleviate pain and promote feelings of well-being during physical activity.
### 🧬 Alpha-synuclein (Neurology)
Definition: A protein that forms abnormal aggregates in the brain, common in Lewy Body Dementia.
### ⚠️ Neuroleptic Sensitivity (Neurology)
Definition: A severe adverse reaction to antipsychotic medications often seen in patients with LBD.
### 🔄 Cognitive Fluctuations (Neurology)
Definition: Spontaneous and rapid changes in alertness, attention, or thinking ability.
### 🌙 REM Sleep Behavior Disorder (Neurology)
Definition: A sleep disorder where individuals physically act out vivid or unpleasant dreams.
### 🧈 Fat-Soluble Vitamins (Nutrition)
Definition: Vitamins A, D, E, and K that require dietary fat for absorption and storage.
### 💧 Water-Soluble Vitamins (Nutrition)
Definition: Vitamins B and C that dissolve in water and require regular intake as they are not stored.
### ➡️ Absorption (Nutrition)
Definition: The process of nutrients moving from the digestive tract into the bloodstream.
### ⚠️ Deficiency (Nutrition)
Definition: A clinically low nutrient level that may impair health or cause specific symptoms.
### 🩺 Multivitamin (Nutrition)
Definition: A supplement containing various vitamins and minerals to support general health.
### ➕ Supplement (Nutrition)
Definition: A product intended to add nutritional value to the diet when food intake is insufficient.
### 🧬 AlphaFold (Health Technology)
Definition: An AI system developed by Google DeepMind to predict complex protein structures.
### 🤖 Generative AI (Healthcare) (Health Technology)
Definition: AI models used to generate text, images, or data summaries to assist clinical workflows.
### ⚠️ AI Hallucination (Health Technology)
Definition: A plausible-sounding but incorrect or fabricated output generated by an AI model.
### 📊 Multimodal Data (Health Technology)
Definition: Integrated data types, such as genomics and imaging, used for comprehensive health insights.
### 🌿 Healthspan (Public Health)
Definition: The period of life spent in good health, free from chronic disease or disability.
### ⚖️ Health Equity (Public Health)
Definition: The fair opportunity for every individual to attain their full health potential.
### 🏘️ Social Determinants of Health (SDOH) (Public Health)
Definition: Non-medical factors like housing and food security that influence health outcomes.
### 🎯 Precision Medicine (Clinical Science)
Definition: Medical care tailored to an individual’s genetic, environmental, and lifestyle profile.
### 🩺 Multi-morbidity (Clinical Science)
Definition: The presence of two or more chronic health conditions in a single individual.
### 💊 Cholinesterase Inhibitors (Medications)
Definition: Drugs that improve cognitive function by increasing acetylcholine levels in the brain.
### 💊 Polypharmacy (Medications)
Definition: The concurrent use of multiple medications, typically five or more, by one patient.
### 🔄 Medicaid (Insurance)
Definition: The cycling of individuals on and off Medicaid due to income or administrative shifts.
### 🦋 Metamorphosis (Psychological Growth)
Definition: A profound transformation in form, function, or understanding. In aging, it often refers to the inner changes that occur as people adapt, grow, and reinterpret their life experiences.
### 🧭 Philosophical Shift (Meaning & Purpose)
Definition: A meaningful change in how a person views life, purpose, or values. Often emerges in later life as priorities evolve and individuals seek deeper meaning and clarity.
### 🦉 Sagacity (Wisdom)
Definition: Deep wisdom gained through experience, reflection, and insight. Sagacity often strengthens with age as individuals integrate lessons learned across a lifetime.
### 💞 Empathy (Relationships & Connection)
Definition: The ability to understand and share the feelings of another person. Empathy supports healthy relationships, emotional well-being, and social connection throughout the lifespan.
### 🌄 Gerotranscendence (Aging Theories)
Definition: A developmental theory describing a natural shift in older adulthood toward greater reflection, inner peace, and a broader, more spiritual or existential perspective.
### 🌿 Parasympathetic Recovery (Body & Nervous System)
Definition: The body’s return to a calm, restorative state after stress, driven by the parasympathetic nervous system. Supports heart health, digestion, emotional regulation, and resilience.
### 🧠 Hepatic Encephalopathy (Liver & Metabolism)
Definition: A brain-related complication of liver disease caused by toxins-especially ammonia-that the liver can no longer clear. Can lead to confusion, sleep changes, irritability, or slowed thinking.
### 💧 Albumin (Liver & Metabolism)
Definition: A major blood protein made by the liver that helps maintain fluid balance, transport hormones, and support circulation. Low levels contribute to swelling and fatigue.
### 💉 Albumin Therapy (Treatments & Procedures)
Definition: An intravenous infusion used to restore albumin levels, stabilize blood pressure, and protect kidney function during complications such as paracentesis or infection.
### 🩸 Esophageal Varices (Digestive System)
Definition: Enlarged veins in the esophagus caused by portal hypertension. These fragile veins can rupture and bleed, requiring monitoring and preventive treatment.
### 🩺 Banding (Treatments & Procedures)
Definition: A procedure where rubber bands are placed around varices to stop bleeding or prevent future bleeding. Treats the veins, not the underlying portal pressure.
### 💊 Beta-Blockers (Medications)
Definition: Medications that lower portal pressure and reduce the risk of variceal bleeding by slowing the heart rate and decreasing blood flow through the portal system.
### 🟢 Compensated Cirrhosis (Liver Disease Stages)
Definition: A stage of cirrhosis where the liver is scarred but still performing enough essential functions to avoid major complications.
### 🔴 Decompensated Cirrhosis (Liver Disease Stages)
Definition: A stage of cirrhosis where the liver can no longer maintain normal function, leading to complications such as ascites, variceal bleeding, jaundice, or encephalopathy.
### 🧪 Insulin (Blood Sugar & Hormones)
Definition: A hormone produced by the pancreas that allows glucose to enter cells for energy. Essential for blood sugar regulation. People with type 1 diabetes require insulin therapy; many with type 2 may also need it.
### 🍬 Glucose (Blood Sugar & Hormones)
Definition: A simple sugar that serves as the body’s primary energy source. Blood glucose levels are tightly regulated by insulin and other hormones. Chronically high levels can damage organs and tissues.
### 📈 CGM (Continuous Glucose Monitor) (Monitoring & Devices)
Definition: A wearable device that continuously tracks glucose levels in the interstitial fluid. Helps detect trends, reduce hypoglycemia risk, and improve diabetes management without frequent fingersticks.
### 🩺 A1C (Monitoring & Devices)
Definition: A lab test that measures the percentage of glycated hemoglobin in the blood. Reflects average blood sugar over 2–3 months. Used to diagnose diabetes and assess long-term control.
### 👁️ Retinopathy (Complications)
Definition: Damage to the retina’s blood vessels caused by diabetes. Can lead to vision loss or blindness. Regular eye exams are essential for early detection and treatment.
### 🧫 Nephropathy (Complications)
Definition: Kidney damage caused by diabetes. Early signs include protein in the urine. Progression can lead to chronic kidney disease or dialysis. Blood pressure and blood sugar control are key to prevention.
### 🥖 Carbohydrates (Nutrition & Lifestyle)
Definition: Macronutrients that include sugars, starches, and fiber. Carbs raise blood sugar and must be balanced with insulin or medications. Found in grains, fruits, vegetables, and sweets.
### 📊 Glycemic Index (Nutrition & Lifestyle)
Definition: A ranking system that shows how quickly carbohydrate-containing foods raise blood sugar. Low-GI foods cause slower, more stable rises and are preferred for diabetes management.
### 💊 Metformin (Medications)
Definition: A first-line oral medication for type 2 diabetes. Lowers blood sugar by reducing liver glucose production and improving insulin sensitivity. Also used in prediabetes and PCOS.
### 🧬 GLP-1 Agonists (Medications)
Definition: Medications that mimic the GLP-1 hormone to stimulate insulin release, suppress appetite, and slow digestion. Used in type 2 diabetes and obesity. Examples include semaglutide and liraglutide.
### ⚠️ Hypoglycemia (Emergency Terms)
Definition: A condition where blood sugar drops below normal. Symptoms include shakiness, confusion, sweating, and fainting. Treated with fast-acting carbohydrates like juice or glucose tablets.
### 🔥 Hyperglycemia (Emergency Terms)
Definition: A condition where blood sugar is too high. Symptoms include thirst, fatigue, blurry vision, and frequent urination. Can lead to diabetic ketoacidosis or long-term organ damage.
### 🥫 Ultra‑processed foods (Food & Nutrition)
Definition: Industrial food products made with additives, flavor enhancers, and minimal whole ingredients.
### 🧂 Sodium sensitivity (Blood Pressure)
Definition: A heightened blood pressure response to dietary salt intake.
### ⚗️ BPA (Chemical Exposures)
Definition: A chemical used in some can linings and plastics that may leach into food.
### 📏 Serving size (Food Labels)
Definition: The labeled portion of food, which may represent only part of the package or can.
### 💧 Fluid retention (Fluid Balance)
Definition: Water buildup in the body often triggered by high sodium intake.
### 🏭 Reformulation (Food Industry)
Definition: An industry process where products are modified to reduce harmful nutrients or additives.
### 🧬 Interleukin-23 (IL-23) (Psoriasis)
Definition: A protein involved in inflammation, targeted by newer biologics.
### 💡 Phototherapy (Psoriasis)
Definition: Treatment using ultraviolet light.
### 🦴 Psoriatic Arthritis (Psoriasis)
Definition: A form of arthritis affecting some people with psoriasis.
### 🧴 Calcineurin Inhibitors (Psoriasis)
Definition: Topical drugs that suppress immune activity.
### ⚡ Hyperproliferation (Psoriasis)
Definition: Excessive cell growth, common in psoriasis.
### 🍅 Nightshades (Nightshades)
Definition: A plant family (Solanaceae) that includes tomatoes, peppers, potatoes, and eggplant.
### ⚗️ Alkaloids (Nightshades)
Definition: Natural defense chemicals in nightshades that may irritate sensitive individuals.
### 🌿 Solanaceae (Nightshades)
Definition: The botanical family that includes nightshade vegetables, fruits, and spices.
### 🌶️ Capsaicin (Nightshades)
Definition: A compound in chili peppers responsible for heat; may irritate sensitive skin or digestion.
### 🫐 Goji Berries (Nightshades)
Definition: A nightshade fruit often marketed for antioxidants; may trigger symptoms in sensitive individuals.
### 🧬 Viral Vectors (Genetics & Biotechnology)
Definition: Viruses engineered to deliver genetic material into cells.
### 🫧 Liposomes (Genetics & Biotechnology)
Definition: Tiny lipid-based spheres used to encapsulate and deliver drugs or genetic material.
### ⚡ Electroporation (Genetics & Biotechnology)
Definition: A technique that uses electrical pulses to temporarily open cell membranes for DNA or RNA entry.
### 🔪 Cas Proteins (Genetics & Biotechnology)
Definition: Enzymes that cut or modify DNA as part of CRISPR gene-editing systems.
### 🧫 CRISPR (Genetics & Biotechnology)
Definition: A gene-editing technology that uses guide RNA and Cas proteins to target specific DNA sequences.
### 🧱 Genetic Engineering (Genetics & Biotechnology)
Definition: The process of modifying an organism’s DNA to change or enhance traits.
### 🌐 Nanoparticles (Genetics & Biotechnology)
Definition: Ultrafine particles used to transport drugs, RNA, or DNA into cells.
### 📦 Delivery Systems (Genetics & Biotechnology)
Definition: Methods used to transport therapeutic molecules into cells or tissues.
### 💉 Microinjections (Genetics & Biotechnology)
Definition: Direct injection of genetic material or tools into individual cells or embryos.
### 📊 Expression Patterns (Genetics & Biotechnology)
Definition: Patterns showing when and where genes are turned on or off in an organism.
### 🧩 Gene Structures (Genetics & Biotechnology)
Definition: The arrangement of exons, introns, and regulatory elements within a gene.
### 🎚️ Regulatory Sequences (Genetics & Biotechnology)
Definition: DNA sequences that control when, where, and how strongly genes are expressed.
### ✂️ Gene-Editing (Genetics & Biotechnology)
Definition: Techniques that modify DNA or RNA to correct, remove, or replace genetic information.
### 🧪 Synthetic Biology (Genetics & Biotechnology)
Definition: An interdisciplinary field that designs and constructs new biological systems or reprograms existing ones.
### 🧠 Genetic Diseases (Genetics & Biotechnology)
Definition: Disorders caused by mutations or abnormalities in an individual's DNA.
### 🧬 Colibactin (Colon Health)
Definition: A genotoxin produced by certain gut bacteria that can damage DNA and increase colon cancer risk.
### 🧪 MakA (Colon Health)
Definition: A protein from Vibrio cholerae that selectively targets and kills colon cancer cells in early research.
### 🧬 ctDNA (Colon Health)
Definition: Fragments of tumor DNA circulating in the bloodstream, used for early cancer detection and monitoring.
### 🧬 Lynch Syndrome (Colon Health)
Definition: A hereditary condition caused by mutations in DNA mismatch repair genes, greatly increasing colon cancer risk.
### 🧪 PIK3CA Mutation (Colon Health)
Definition: A mutation in the PIK3CA gene that may predict strong response to low-dose aspirin therapy.
### 🧬 Liquid Biopsy (Colon Health)
Definition: A minimally invasive test that detects tumor DNA in blood, often before tumors appear on scans.
### 🧫 Adenomatous Polyp (Colon Health)
Definition: A type of colon polyp with a higher likelihood of becoming cancerous if untreated.
### 🔬 Dysplasia (Colon Health)
Definition: A measure of how abnormal colon cells appear under a microscope, used to estimate cancer risk.
### 🧬 Familial Adenomatous Polyposis (FAP) (Colon Health)
Definition: A hereditary condition causing hundreds of polyps in the colon, often requiring early preventive surgery.
### 🧪 CEA (Carcinoembryonic Antigen) (Colon Health)
Definition: A tumor marker sometimes elevated in colon cancer, used to monitor treatment response.
### 🧫 Serrated Pathway (Colon Health)
Definition: A type of colon cancer that develops from serrated polyps, often linked to specific genetic mutations.
### 🧬 Mismatch Repair Testing (MMR) (Colon Health)
Definition: A genetic test panel that checks for inherited mutations linked to colon cancer risk.
### ⚙️ Apoptosis (Cancer Biology)
Definition: Programmed cell death - the built‑in 'self‑destruct' mechanism that MakA triggers in cancer cells.
### 🧪 Cytotoxin (Cancer Biology)
Definition: A substance that is toxic to specific cells. In this context, a 'smart' toxin designed to selectively kill tumor cells.
### 🔧 Polypectomy (Screening & Prevention)
Definition: The removal of a polyp during colonoscopy - a simple procedure that prevents cancer before it starts.
### 🔥 Inflammation Load (Psoriasis)
Definition: The total amount of inflammation affecting the body at one time. Smoking can increase this load, which may influence psoriasis symptoms.
### ⚠️ Trigger Stacking (Psoriasis)
Definition: When multiple small triggers-such as stress, smoking, or poor sleep-combine and make psoriasis flares more likely.
### 🩸 Circulation Slowdown (Psoriasis)
Definition: Reduced blood flow that can make skin appear dull or irritated. Smoking is known to contribute to this effect.
### 🌡️ Psoriatic Irritation (Psoriasis)
Definition: The redness, scaling, and discomfort associated with psoriasis, often influenced by inflammation and environmental triggers.
### 💬 Stress‑Linked Flares (Psoriasis)
Definition: Psoriasis flare‑ups that occur or worsen during periods of emotional or physical stress.
### 🍅 Nightshades (Foods)
Definition: A vegetables family including tomatoes, peppers, and eggplants that some people report sensitivity to.
### 🍞 Refined Carbohydrates (Foods)
Definition: Processed grains in white bread and pasta that may affect inflammation for some individuals.
### 🍬 Added Sugars (Foods)
Definition: Sugars added during processing that may influence inflammation in some people.
### 🌻 Seed Oils (Foods)
Definition: Oils such as soybean, corn, and sunflower oil that some people believe affect inflammation.
### 🧀 Dairy Sensitivity (Foods)
Definition: A reaction some people experience to milk or cheese that may affect joint symptoms.
### 🥓 Processed Meats (Foods)
Definition: Meats preserved with salt or additives that may influence inflammation.
### 📦 Ultra-Processed Foods (Foods)
Definition: Highly processed packaged foods that some people find worsen arthritis symptoms.
### ⚗️ Artificial Sweeteners (Ingredients)
Definition: Low-calorie sweeteners that some individuals report sensitivity to.
### 🔥 Inflammation (Health)
Definition: The body's natural response to injury or irritation, which can affect joints.
### 🚫 Trigger Foods (Diet)
Definition: Foods that may worsen symptoms for some individuals with arthritis.
### 🛌 Psoriasis Sleep Disruption (Psoriasis)
Definition: Difficulty falling or staying asleep due to itching, pain, or emotional stress linked to psoriasis.
### 🌙 Inflammatory Sleep Cycle (Psoriasis)
Definition: A pattern where systemic inflammation interferes with deep sleep, often seen in chronic conditions like psoriasis.
### 🌡️ Nocturnal Itch Spike (Psoriasis)
Definition: Increased itching during nighttime hours, commonly reported by people with psoriasis or eczema.
### 😣 Restless Skin Sensation (Psoriasis)
Definition: A feeling of skin discomfort or agitation that makes it hard to relax or sleep, often linked to inflammation.
### ⏰ Sleep-Linked Flare Pattern (Psoriasis)
Definition: Psoriasis flares that worsen after poor sleep or during periods of sleep disruption.
### 💉 Biologics (Psoriasis Treatments)
Definition: Advanced medications made from living cells that target specific parts of the immune system involved in psoriasis. Often used when topical treatments or light therapy are not enough.
### 🧬 TNF Inhibitors (Psoriasis Treatments)
Definition: A class of biologics that block tumor necrosis factor (TNF), a protein involved in inflammation. Commonly used for both psoriasis and psoriatic arthritis.
### ⚡ IL-17 Inhibitors (Psoriasis Treatments)
Definition: Biologic medications that target the IL‑17 pathway, which plays a role in plaque formation. Known for fast skin‑clearing effects in many patients.
### 🔒 IL-23 Inhibitors (Psoriasis Treatments)
Definition: Biologics that block the IL‑23 protein, an upstream driver of inflammation. Often associated with long-lasting results and fewer injections.
### 💊 JAK Inhibitors (Psoriasis Treatments)
Definition: Oral medications that work inside immune cells to interrupt inflammatory signals. Sometimes used when injections are not preferred.
### ♻️ Biosimilars (Psoriasis Treatments)
Definition: Medications designed to be highly similar to an existing biologic. They offer comparable effectiveness and may be used when insurance coverage changes.
### 🏷️ Manufacturer Assistance Programs (Psoriasis Treatments)
Definition: Programs offered by drug manufacturers to help patients access medications when insurance coverage changes or costs become high.
### 🌊 Laminar Flow (Vascular System)
Definition: Smooth, straight-line blood flow-like a quiet river. This is the goal of Stress Mastery and proper medication: keeping blood moving without creating the friction that leads to clots.
### 🌪️ Turbulent Flow (Vascular System)
Definition: Disrupted, swirling blood flow caused by high pressure or vessel narrowing. This 'rough water' can damage vessel walls and is a primary risk factor during the 48-hour TIA window.
### 🩸 Portal Hypertension (Vascular System)
Definition: Increased blood pressure in the portal vein system-the liver’s plumbing. When this pressure is high, it can influence the entire systemic bridge, including brain circulation.
### 🧵 Vasoconstriction (Vascular System)
Definition: The narrowing of blood vessels. Stress and high cortisol cause this, 'kinking the hose' and forcing the heart to work harder, which spikes pressure in sensitive brain vessels.
### 🧠 Neuroplasticity (Brain & Nervous System)
Definition: The brain's ability to reorganize itself. Pillar 2 (Movement) encourages this, helping the brain stay resilient even if a TIA or minor vascular event occurs.
### ⚠️ ISR (Neuroscience)
Definition: The Integrated Stress Response, a cellular safety mechanism that becomes overactive in Alzheimer’s, triggering toxic lipid production.
### 🧬 Proteostasis (Cell Biology)
Definition: The balance of protein creation, folding, and clearance. Disrupted proteostasis contributes to neurodegeneration.
### 🧠 Parkin (Neurodegeneration)
Definition: A protein that helps clear damaged mitochondria. Impaired Parkin activity is linked to Parkinson’s and Alzheimer’s.
### 🌑 Dark Microglia (Neuroscience)
Definition: A stress-induced microglial subtype associated with synapse loss, inflammation, and Alzheimer’s progression.
### 🧩 Proteotoxicity (Neuroscience)
Definition: Cellular damage caused by misfolded or aggregated proteins, common in Alzheimer’s and Parkinson’s.
### 🧩 Psoriatic Arthritis (PsA) (Bone and Joint Health)
Definition: A chronic inflammatory arthritis linked to psoriasis, involving joints, tendons, and the immune system.
### 📝 PEST Screening Tool (Screening & Assessment)
Definition: A five‑question screening tool used to detect early signs of psoriatic arthritis in people with psoriasis.
### 📑 GRAPPA (Clinical Guidelines)
Definition: An international consortium that develops evidence‑based treatment recommendations for psoriasis and psoriatic arthritis.
### 🖐️ Dactylitis (Bone and Joint Health)
Definition: Diffuse swelling of an entire finger or toe caused by inflammation of joints, tendons, and soft tissues.
### 🎯 Enthesitis (Bone and Joint Health)
Definition: Inflammation where tendons or ligaments attach to bone, contributing to pain and stiffness in psoriatic arthritis.
### 🧍♂️ Axial Psoriatic Arthritis (Bone and Joint Health)
Definition: A subtype of psoriatic arthritis affecting the spine and sacroiliac joints, causing inflammatory back pain and stiffness.
### 🔥 GERD (Gastroesophageal Reflux Disease) (Digestive Health)
Definition: A chronic condition where stomach acid repeatedly flows back into the esophagus, causing irritation.
### 🌶️ Heartburn (Digestive Health)
Definition: A burning sensation in the chest caused by acid moving upward into the esophagus.
### 🔒 Lower Esophageal Sphincter (LES) (Digestive Health)
Definition: A muscle ring at the bottom of the esophagus that prevents stomach acid from flowing upward.
### 🗣️ Silent Reflux (LPR) (Digestive Health)
Definition: Reflux that affects the throat and voice box, often without classic heartburn symptoms.
### ⬆️ Hiatal Hernia (Digestive Health)
Definition: A condition where part of the stomach pushes upward through the diaphragm, increasing reflux risk.
### 💊 Proton Pump Inhibitors (PPIs) (Digestive Health)
Definition: A class of medications that reduce stomach acid production to help manage GERD symptoms.
### 📋 Medicare Advantage (Part C) (Medicare)
Definition: A bundled Medicare plan (Part C) offered by private insurers, combining hospital, medical, and often drug coverage with extra benefits.
### 💊 Formulary (Medicare)
Definition: The list of prescription drugs covered by a Medicare Advantage or Part D plan. Each plan has its own formulary and drug tiers.
### 💰 Out-of-Pocket Maximum (Medicare)
Definition: The highest amount you’ll pay in a year for covered services under a Medicare Advantage plan. Original Medicare does not have this cap.
### 📝 Prior Authorization (Medicare)
Definition: A requirement that your doctor or plan must get approval before a service is covered. Common in Medicare Advantage plans.
### 🎁 Supplemental Benefits (Medicare)
Definition: Extra services offered by Medicare Advantage plans, such as dental, vision, hearing, fitness, transportation, and OTC allowances.
### 🔄 PPO (Preferred Provider Organization) (Medicare)
Definition: A type of Medicare Advantage plan that allows you to use doctors and hospitals outside the plan’s network, often at a higher cost.
### 🔒 HMO (Health Maintenance Organization) (Medicare)
Definition: A type of Medicare Advantage plan that requires you to use doctors and hospitals within the plan’s network for coverage.
### 📆 Annual Enrollment Period (AEP) (Medicare)
Definition: The annual window (October 15 – December 7) when you can change Medicare Advantage or Part D plans.
### 🔁 Medicare Advantage Open Enrollment (Medicare)
Definition: The January 1 – March 31 window when you can switch Medicare Advantage plans or return to Original Medicare.
### ⚡ Creatine (Muscle Energetics)
Definition: A naturally occurring compound that helps muscles recycle quick-burst energy for strength, balance, and daily movement.
### 🔋 ATP (Adenosine Triphosphate) (Muscle Energetics)
Definition: The primary energy molecule used by cells for movement, muscle contraction, and metabolic activity.
### 💥 Phosphocreatine (Muscle Energetics)
Definition: A stored form of quick-release energy in muscle cells that powers short, functional movements like standing or climbing stairs.
### 🔧 Muscle Energetics (Muscle Energetics)
Definition: The system that governs how muscles create, store, and use energy for strength, mobility, and daily function.
### 🛡️ HMB (Beta-Hydroxy Beta-Methylbutyrate) (Healthy Aging Biology)
Definition: A metabolite of leucine that helps reduce muscle breakdown, especially during inactivity or illness.
### 🥚 Leucine Threshold (Healthy Aging Biology)
Definition: The minimum amount of leucine needed in a meal to trigger muscle protein synthesis, typically around 2.5–3 grams.
### 📉 Anabolic Resistance (Healthy Aging Biology)
Definition: The reduced ability of aging muscle to respond to protein, requiring higher and more targeted protein doses to stimulate growth.
### 🏃 Fast-Twitch Muscle Fibers (Healthy Aging Biology)
Definition: Type II muscle fibers responsible for power, balance, and quick movements; they decline earlier and faster with age.
### 🔬 mTORC1 (Healthy Aging Biology)
Definition: A cellular growth switch that increases protein synthesis when activated by amino acids, especially leucine.
### ♻️ Autophagy (Healthy Aging Biology)
Definition: The cell’s cleanup and recycling system that removes damaged proteins and mitochondria, supporting longevity and metabolic health.
### 🕶️ UV Protection (Eye Health)
Definition: Shielding the eyes from ultraviolet light to reduce the risk of cataracts and retinal damage.
### 🩺 Ambient Scribe (Vein Health)
Definition: An AI-powered tool that 'listens' to a consultation to generate medical notes, allowing the doctor to focus on the patient rather than a screen.
### 🩺 Bio-Adhesive (Vein Health)
Definition: Often called 'Medical Glue' (like VenaSeal), this is a non-thermal 2026 standard for sealing varicose veins without the use of heat or multiple injections.
### 🩺 Chronic Venous Insufficiency (CVI) (Vein Health)
Definition: The medical term for a condition where the leg veins don't allow blood to flow back up to the heart effectively, often leading to varicose veins.
### 🩺 Duplex Ultrasound (Vein Health)
Definition: A diagnostic test that uses high-frequency sound waves to visualize the structure of the veins and the speed/direction of blood flow.
### 🩺 Endovenous Laser (EVLT) (Vein Health)
Definition: A procedure that uses a tiny laser fiber to deliver heat (thermal energy) to the vein wall, causing it to collapse and eventually be absorbed by the body.
### 🩺 Micro-Phlebectomy (Vein Health)
Definition: A minimally invasive procedure where a doctor removes varicose veins through tiny 'micro-incisions' that typically do not require stitches.
### 🩺 Post-Quantum Cryptography (Vein Health)
Definition: In 2026, the new security standard used by health clinics to protect your vascular records from being decrypted by future advanced computers.
### 🩺 Reflux (Vein Health)
Definition: The clinical term for blood flowing in the wrong direction (backward) because of a failed valve.
### 🩺 Spider Veins (Vein Health)
Definition: Smaller, red or purple veins that sit closer to the skin’s surface. While often cosmetic, they can be a 'warning light' for deeper venous issues.
### 🩺 Tumescent Anesthesia (Vein Health)
Definition: A specialized local anesthetic used in older thermal procedures (like EVLT) that requires multiple needle sticks around the target vein.
Normal Aging🧠Age-related changes such as occasional forgetfulness or slower recall that do not significantly interfere with daily life.
Dementia🧠A progressive decline in memory, thinking, and daily functioning that is not a normal part of aging.
Mild Cognitive Impairment (MCI)🧠A stage between normal aging and dementia with noticeable cognitive changes but mostly preserved independence.
Alzheimer’s Disease🧠The most common cause of dementia, often beginning with Mild Cognitive Impairment and progressing over time.
Lecanemab💉An FDA-approved monoclonal antibody that reduces amyloid plaques and slows early Alzheimer’s disease progression.
Donanemab💉An investigational monoclonal antibody that targets amyloid plaques and has shown benefit in early Alzheimer’s disease trials.
Amyloid Plaques🔬Abnormal protein clumps in the brain associated with Alzheimer’s disease and targeted by drugs like lecanemab and donanemab.
Medicare Annual Wellness Visit📋A yearly Medicare visit that can include questions or screening for memory and cognitive changes.
Muscle-Based Ammonia Detox🧠The process where skeletal muscle compensates for impaired liver detoxification by removing ammonia from the bloodstream.
Low BCAA State🧬A metabolic imbalance in cirrhosis where branched-chain amino acids are depleted due to increased ammonia detoxification demands.
Catabolic Overnight Shift🌜The nighttime metabolic pattern in cirrhosis where the body rapidly breaks down muscle due to limited glycogen stores.
Energy Partitioning Failure⚙️A disruption in how the body allocates carbohydrates, fats, and proteins, common in advanced liver disease.
Inflammation-Driven Muscle Loss🔥Muscle wasting caused by chronic inflammation, altered amino acid balance, and impaired liver function.
You may also enjoy
2 minute read
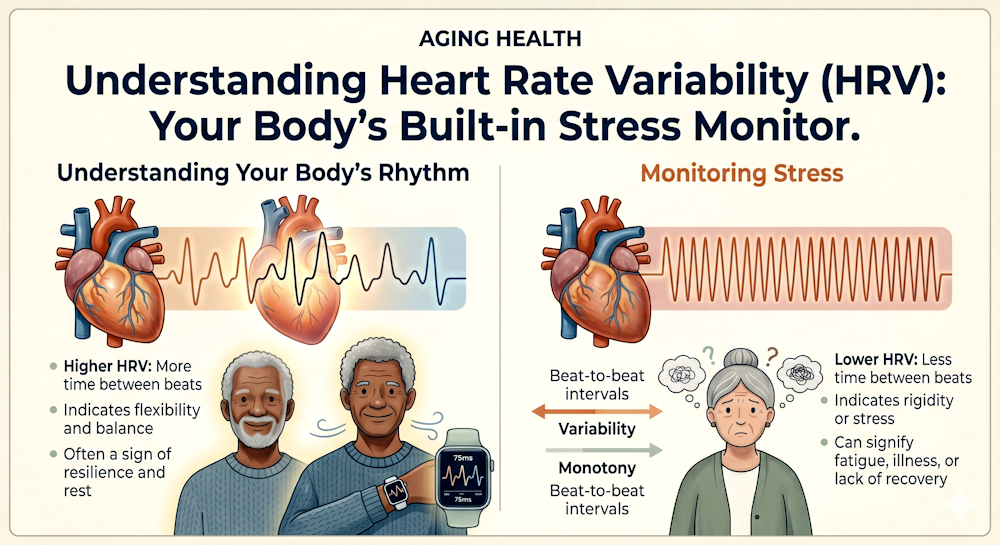
As an independent researcher, I often examine data that can provide a window into systemic health. While many metrics require complex clinical tests, Heart R...
2 minute read
Building muscle as we age is not just a physical challenge—it’s a psychological one. Explore how mindset shapes strength outcomes for seniors.
2 minute read
Navigating medical care often feels like learning a second language. Between the acronyms and the ranges, a simple blood work report can look more like a mat...
3 minute read
The National Institute on Aging (NIA): Why It Matters in 2026
 Understanding the structural differences between these two viruses helps scientists develop targeted vaccines and treatments.
Understanding the structural differences between these two viruses helps scientists develop targeted vaccines and treatments.