Psoriasis: Personal Advocacy and Systemic Research
A 4-year journey through plaque psoriasis and the transition to psoriatic arthritis, combined with a guide to navigating the biologic paywall.
Living Research: My 4-Year Psoriasis Journey
I don't just study psoriasis; I live it. For over four years, I have managed flare-ups primarily on my feet and legs. Recently, my journey took a turn as I began developing symptoms of Psoriatic Arthritis—a challenging progression where the immune system moves from the skin to the joints.
The Cost of Care: Two years ago, when my insurance stopped covering Humira, I turned to AbbVie Assist. Without manufacturer patient assistance, the biologic therapy that keeps my symptoms stable would be inaccessible. This guide combines personal advocacy with clinical data to help you navigate both the physical and financial hurdles of this condition.
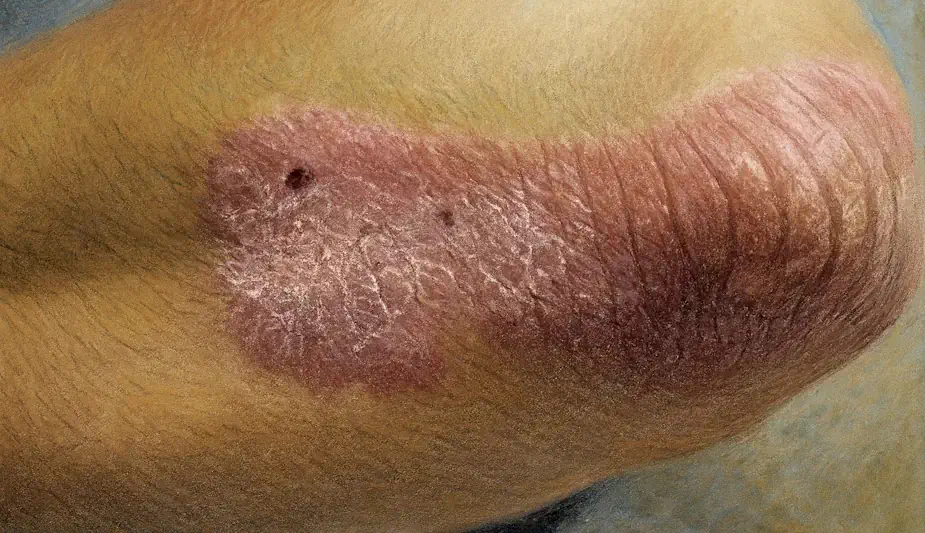 Figure 1: Psoriasis is a systemic autoimmune disorder; early detection and intervention are essential for preventing joint damage.
Figure 1: Psoriasis is a systemic autoimmune disorder; early detection and intervention are essential for preventing joint damage.
What Drives Psoriasis?
Psoriasis is marked by thick, scaly skin patches resulting from an overactive immune system. While genetics play a role (over 80 genes have been identified), environmental triggers—such as stress, infections, and weather—are often what set the “immune fire.”
- Immune Misfire: The body mistakenly attacks healthy skin cells, accelerating their growth cycle from 28 days down to just 3 or 4 days.
- Hereditary Links: Carrying the genes doesn’t guarantee a diagnosis; it’s the “gene-environment” handshake that matters.
Symptoms Beyond the Surface
- Plaques: Red, raised patches with silvery scales (found on elbows, knees, and scalp).
- Nail Pitting: Discoloration or separation from the nail bed (onycholysis).
- Scalp Flaking: Affects 50% of patients and is often mistaken for simple dandruff.
- Emotional Impact: The visible nature of the disease can lead to social withdrawal, anxiety, and depression.
The Joint Connection: Psoriatic Arthritis (PsA)
About 30% of patients will progress to PsA. Watch for these clinical “red flags”:
- Dactylitis: “Sausage-like” swelling of fingers or toes.
- Enthesitis: Pain at the heels or elbows where tendons meet bone.
- Morning Stiffness: Joint pain that requires 30+ minutes of movement to ease.
Navigating the Biologic “Paywall”
Biologics can cost over $5,000 per month. If you are struggling with access, consider these resources:
| Resource | Function | Target Audience |
|---|---|---|
| Patient Assistance (PAP) | $0 medications directly from manufacturers (e.g., AbbVie Assist). | Uninsured or under-insured. |
| Copay Cards | Reduces pharmacy out-of-pocket costs to as low as $5. | Commercial insurance patients. |
| Step Therapy | The “Fail First” rule required by many insurance plans. | New diagnoses. |
Nightshades and Inflammation
While there is no scientific consensus, a 2017 survey showed that 52.1% of patients saw improvement by removing nightshades (tomatoes, potatoes, eggplants, and peppers). These plants contain alkaloids that may irritate the gut lining in sensitive individuals.
March 2026 Clinical Update: Systemic Management
Psoriasis is now viewed as a systemic inflammatory event, not just a skin condition. Current clinical targets for stabilization include:
- Metabolic Support: High-quality protein intake is essential to maintain skin cell turnover and lean muscle mass: \(1.2\text{--}1.6 \text{ g/kg of body weight}\)
- Inflammatory Control: Managing psoriasis is functionally similar to managing liver and heart health—it requires reducing “systemic fire” through both biologics and lifestyle.
📖 Glossary
- Hyperproliferation: The excessive growth of skin cells.
- Biologics: Medications targeting specific proteins (like IL-17 or IL-23).
- Phototherapy: The use of specific UV light wavelengths to slow cell growth.
- JAK Inhibitors: Oral medications that block immune signaling switches.