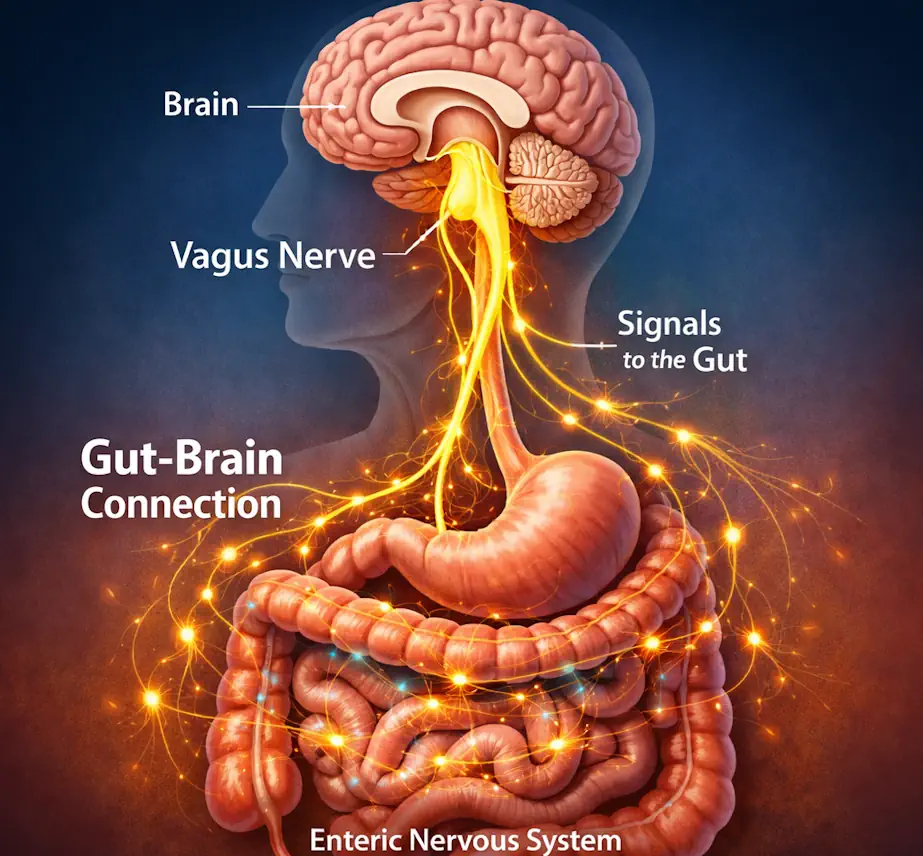
The Vagus Highway: How the Gut-Brain Axis Drives Neurodegeneration
Why 2026 clinical research treats the gut as the 'Ground Zero' for Lewy Body Dementia and Parkinson's Disease.
The 2026 ‘Bottom-Up’ Consensus Emerging research suggests that the abnormal proteins found in Lewy Body Dementia (LBD) may actually originate in the enteric nervous system—the “brain in the gut”—before traveling up the vagus nerve to the brain.
Figure 1: The Vagus nerve acts as a bidirectional highway, carrying alpha-synuclein “seeds” from the gut to the brain.
Ground Zero: The Enteric Origin Hypothesis
For decades, we treated neurodegeneration as a “head-only” problem. In 2026, we now recognize the Enteric Origin Hypothesis. This theory posits that chronic gut inflammation causes alpha-synuclein (a specific protein) to misfold in the intestinal lining.
Once misfolded, these proteins act like “seeds,” traveling up the Vagus Nerve—the body’s longest cranial nerve—until they reach the brainstem and eventually the cognitive centers.
The “Leaky Gut” and the Blood-Brain Barrier
A “leaky gut” (intestinal permeability) is more than a digestive issue. When the tight junctions of the gut wall weaken, pro-inflammatory molecules called Lipopolysaccharides (LPS) enter the bloodstream.
This triggers a systemic “fire” that eventually weakens the Blood-Brain Barrier (BBB). Once the BBB is compromised, the brain’s specialized immune cells (microglia) go into overdrive, leading to the neuro-inflammation seen in LBD and Alzheimer’s.
Clinical Targets: Managing the Axis
To protect the brain, we must stabilize the gut. In 2026, patient advocacy focuses on three primary clinical markers:
1. Akkermansia Muciniphila
This “keystone” bacteria strengthens the mucus lining of the gut. Low levels are a hallmark of early-stage neurodegeneration.
2. Short-Chain Fatty Acids (SCFAs)
Produced when healthy gut bacteria ferment fiber, SCFAs like Butyrate serve as direct fuel for brain-protective cells.
3. GLP-1 Protection
Beyond weight loss, GLP-1 therapies (like Ozempic or Mounjaro) are showing promise in 2026 for their ability to reduce gut-wall inflammation, potentially slowing the “seeding” of toxic proteins to the brain.
🍽️ The Gut-Brain Protection Diet
| Nutrient | Clinical Role | 2026 Recommendation |
|---|---|---|
| High-Quality Protein | Combats Sarcopenia & supports cell repair | 1.2 – 1.5 g/kg daily |
| Resistant Starch | Feeds Butyrate-producing bacteria | Cooked/Cooled potatoes & legumes |
| Polyphenols | Reduces oxidative “fire” in the gut | Green tea, EVOO, Blueberries |
Researcher Tip: Managing the Gut-Brain axis is the reason blood pressure targets for seniors have tightened. Keeping systemic BP <130/80 mmHg protects the delicate micro-vessels in both the gut and the brain.
Conclusion
The gut is no longer just for digestion; it is the frontline of cognitive longevity. By prioritizing gut barrier integrity and microbiome diversity, we can move from “managing symptoms” to “interrupting the pathway” of neurodegeneration.
Sources & Further Reading
- Journal of Neuroinflammation (2025): Alpha-synuclein transport via the Vagus Nerve.
- Gut-Brain Consortium (2026): Clinical guidelines for microbiome support in LBD.
- Aging Health Research: Understanding LBD Symptoms & Care